Specialty Dental Services in Gilbert, AZ

Why race across town to dentists you don’t know? We provide comprehensive, specialized dental care in one familiar place.

Endodontics is a specialized branch of dentistry that deals with the complex structures found inside the teeth. The Greek word “Endodontics” literally means “inside the tooth” and relates to the tooth pulp, tissues, nerves, and arterioles. Endodontists receive additional dental training after completing dental school to enable them to perform both complex and simple procedures, including root canal therapy.
Historically, a tooth with a diseased nerve would be removed immediately, but endodontists are now able to save the natural tooth in most cases. Generally, extracting the inner tooth structures, then sealing the resulting gap with a crown restores health and functionality to damaged teeth.
Signs and symptoms of endodontic problems:
- Inflammation and tenderness in the gums.
- Teeth that are sensitive to hot and cold foods.
- Tenderness when chewing and biting.
- Tooth discoloration.
- Unexplained pain in the nearby lymph nodes.
Reasons for Endodontic Treatment
Endodontic treatment (or root canal therapy) is performed to save the natural tooth. In spite of the many advanced restorations available, most dentists agree that there is no substitute for healthy, natural teeth.
Here are some of the main causes of inner tooth damage:
Bacterial infections – Oral bacteria is the most common cause of endodontic problems. Bacteria invade the tooth pulp through tiny fissures in the teeth caused by tooth decay or injury. The resulting inflammation and bacterial infection jeopardize the affected tooth and may cause an abscess to form.
Fractures and chips – When a large part of the surface or crown of the tooth has become completely detached, root canal therapy may be required. The removal of the crown portion leaves the pulp exposed, which can be debilitating painful and problematic.
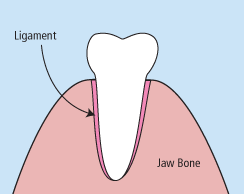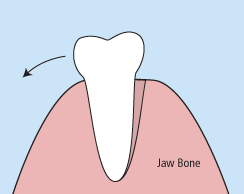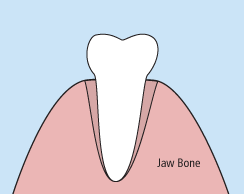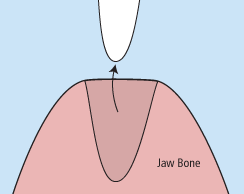
Injuries – Injuries to the teeth can be caused by a direct or indirect blow to the mouth area. Some injuries cause a tooth to become luxated or dislodged from its socket. Root canal therapy is often needed after the endodontist has successfully stabilized the injured tooth.
Removals – If a tooth has been knocked clean out of the socket, it is important to rinse it and place it back into the socket as quickly as possible. If this is impossible, place the tooth in special dental solution (available at pharmacies) or in milk. These steps will keep the inner mechanisms of the tooth moist and alive while emergency dental treatment is sought. The tooth will be affixed in its socket using a special splint, and the endodontist will then perform root canal therapy to save the tooth.
What does an endodontic procedure involve?
Root canal therapy usually takes between one and three visits to complete. Complete X-rays of the teeth will be taken and examined before the treatment begins.
Initially, a local anesthetic will be administered, and a dental dam (protective sheet) will be placed to ensure that the surgical area remains free of saliva during the treatment. An opening will be created in the surface of the tooth, and the pulp will be completely removed using small handheld instruments.
The space will then be shaped, cleaned, and filled with gutta-percha. Gutta-percha is a biocompatible material that is somewhat similar to rubber. Cement will be applied on top to ensure that the root canals are completely sealed off. Usually, a temporary filling will be placed to restore functionality to the tooth prior to the permanent restoration procedure. During the final visit, a permanent restoration or crown will be placed.
If you have questions or concerns about endodontic procedures, please contact our office.
No one wants to lose their teeth, but sometimes it is necessary to undergo an extraction to restore and maintain the health of your smile. Extractions are never your dentist’s first choice, but in certain situations, the preservation of your oral health may be dependent on it.
Reasons Why Tooth Extractions Are Necessary
e always do everything we can to help patients keep their natural teeth, but sometimes it isn’t a viable option. Here are a few reasons why a tooth extraction may be necessary to restore your overall dental health and function:
- There is severe damage or decay to the tooth that is irreparable.
- To allow for a patient to undergo orthodontic treatment.
- For ensuring long-term success with a restoration, like a denture.
- When a primary tooth won’t fall out on its own.
- If a tooth is impacted and unable to erupt properly.
Ultimately, by extracting problematic teeth, future infections and other oral health issues are significantly less likely to occur.
Wisdom Teeth Extractions
Wisdom teeth are types of molars found in the very back of your mouth. They usually appear in the late teens or early twenties, but may become impacted (fail to erupt) due to lack of room in the jaw or angle of entry. When a wisdom tooth is impacted, it may need to be removed. If it is not removed, you may develop gum tenderness, swelling, or even severe pain. Impacted wisdom teeth that are partially or fully erupted tend to be quite difficult to clean and are susceptible to tooth decay, recurring infections, and even gum disease.
Wisdom teeth are typically removed in the late teens or early twenties because there is a greater chance that the teeth’s roots have not fully formed and the bone surrounding the teeth is less dense. These two factors can make extraction easier as well as shorten the recovery time.
In order to remove a wisdom tooth, your dentist first needs to numb the area around the tooth with a local anesthetic. Since the impacted tooth may still be under the gums and embedded in your jaw bone, your dentist will need to remove a portion of the covering bone to extract the tooth. In order to minimize the amount of bone that is removed with the tooth, your dentist will often “section” your wisdom tooth so that each piece can be removed through a small opening in the bone. Once your wisdom teeth have been extracted, the healing process begins. Depending on the degree of difficulty related to the extraction, healing time varies. Your dentist will share with you what to expect and provide instructions for a comfortable, efficient healing process.
The Process of Removing a Tooth
Teeth are generally removed by either pulling or surgical extraction. Teeth can only be “pulled” when they have fully emerged from the gumline. In this case, we will start by numbing the area around your tooth and use a clasping tool to shift the tooth around until it breaks away from the gumline. If pulling isn’t a possibility, the tooth will need to be surgically extracted. For this procedure, a small incision is made into your gum tissue to allow us the ability to reach enough of your tooth to fully remove it.
To determine which extraction method would be necessary for you, come see us for a consultation where we can evaluate your smile. In the process of discussing the extraction, we will also talk about necessary tooth replacement options to prevent future oral health issues as a result of tooth loss.
Tooth Extraction Aftercare
Before you leave the practice, we will provide you with a specific aftercare plan to help you stay comfortable and avoid complications. While every case is different, here are some steps that we will generally recommend for optimal recovery:
- Take recommended over-the-counter and prescribed medications as directed
- Rinse with saltwater 24 hours after your procedure
- Avoid using tobacco products until your mouth has healed
- Do not drink using a straw
- Elevate your head while sleeping
- Get plenty of rest
- Apply a cold compress to reduce swelling and discomfort
- Stay away from hard, crunchy, and sticky foods
Put Your Mind At Ease With Sedation Dentistry

At the Smiles at San Tan Ranch dental office, we provide the opportunity for relaxation and sedation dentistry.
Most people fear the anxiety or pain that they may experience while they are having their dental work done. Sedation Dentistry allows you the opportunity to be in a pain free environment while we do all your dental work.
What is Sedation Dentistry?
One of the major reasons people avoid going to the dentist is because they are afraid. Sedation dentistry can change all of that for you by providing a relaxing environment to ensure your safety.
Smiles at San Tan Ranch holds a state permit for sedation that offers nitrous oxide, oral conscious sedation and IV sedation to give you the sedation choice that works best for you.
Regardless of which type of sedation you receive, you’ll need a numbing medication, at the site where our dentist is working in your mouth to relieve any possible pain from the procedure.
It is important to have a responsible caregiver accompany you to the dental office for the procedure, and drive you home. Pick someone you like and trust because we prefer they stay with you for an additional two to four hours at home.
In most cases we are able to handle all your dental concerns in one single visit so all you have to do is keep up your regular preventative maintenance schedule.
Minimally Invasive Periodontal Gum Therapy

The word periodontal means “around the tooth”. Periodontal disease attacks the gums and the bone that support the teeth. Your mouth is filled with bacteria. When bacteria are not disrupted on a regular basis, a plaque, or a sticky film of bacteria, debris and saliva form on the teeth and under the gum line. If plaque is not thoroughly removed each day, it becomes mineralized and turns into calculus (tartar). This build up on the tooth and root surface become rough and harbor the harmful bacteria of the mouth which begins to destroy the gums and bone. Once calculus has formed your toothbrush will not removed the hardened substance and a professional dental cleaning is required to remove the harmful build up.
Periodontal disease is characterized by red, swollen, and bleeding gums; although not all symptoms need to be present for a diagnosis of periodontal disease.
Four out of five people have some level periodontal disease and don’t know it! Most people are not aware of the condition because the disease is usually painless in the early stages. If your gums are bleeding, this is not normal and is a sign of disease in your mouth.
Good oral hygiene, a balanced diet, and regular dental visits can help reduce your risk of developing periodontal disease. As well as, genetics and your overall health can play a role in periodontal disease progression.

Sleep Apnea is abnormal pauses in breathing while sleeping. During these pauses, the brain, and the rest of the body, may not get enough oxygen.
Central sleep apnea: Unlike OSA, the airway is not blocked, but the brain fails to signal the muscles to breathe due to instability in the respiratory control center.
Sleep Apnea And Your Health
When sleep apnea goes untreated, it can have far-reaching effects on every facet of a person’s health. For instance, sleep apnea has been linked to cardiovascular disorder, mental health problems, stroke, and hypoxemia (low oxygen levels in the blood).
The reason sleep apnea affects the entire body is because it causes sleep deprivation, affects the natural rhythm of air intake, and disrupts the body’s ability to rest and rejuvenate tissues during sleep.
Affects of Sleep Apnea On Your Oral Health
Sleep apnea has been shown to have a negative impact on your teeth and oral health too. Issues that can be caused by sleep apena include:
- Cracked or worn teeth: Grinding or clenching your teeth while you sleep—a condition called bruxism—is more common in people who have sleep apnea. Over time, grinding of the teeth can can cause tooth sensitivity, and even cracked, chipped, or damaged teeth.
- Jaw pain: Sleep apnea is associated with chronic pain disorders, including jaw pain like TMJ or TMD. If it hurts to open and move your jaw bones, you may have one of these conditions.
- Higher risk of developing cavities: People who have sleep apnea are likelier to breathe through their mouths—which can dry out protective saliva and lead to more tooth decay. As a result, you may be at a higher risk for enamel erosion and cavities.
Being diagnosed and treating your sleep apnea can reduce or sometimes even eliminate these dental issues. Talk to your dentist to find out the best treatment plan for you.
Signs And Symptoms of Sleep Apnea
OSA produces symptoms and signs that may be noticed by a sleeper or his or her bed partner. In many instances, OSA causes a patient to gasp for air during sleep or snore loudly. When waking, people with sleep apnea tend to experience dry mouth, headaches, and grogginess. Fatigue and malaise are common, too – even after a person has what they think is a full night’s sleep. Sleep apnea can cause memory loss and depression as well as raised blood pressure.
Is Sleep Apnea Dangerous?
Sleep Apnea is a serious sleep disorder and can be dangerous, but is treatable in most cases.
What Treatment is Available For Sleep Apnea?
Oral appliance therapy is an effective treatment option for snoring and obstructive sleep apnea. Oral appliance therapy is an effective treatment option for snoring and obstructive sleep apnea. Oral appliance therapy should be provided by a qualified dentist who has technical skill and knowledge in dental sleep medicine.
How Sleep Apnea Appliances Work
In the past, obstructive medical equipment or invasive surgeries were used to treat OSA. For instance, CPAP (continuous positive airway pressure) therapy was used during sleep to keep airways open by emitting a constant stream of air. While this was effective, the bulky and loud machinery affected patients’ abilities to sleep comfortably.
To help promote comfort, our dentist may recommend the use of a custom oral appliance. This appliance is made from soft materials and is worn in the mouth during sleep. By slightly repositioning the lower mandible (jaw) forward, the appliance can prevent soft oral tissues from collapsing into airways during sleep.
Temporomandibular Disorder (TMD)
Millions of Americans suffer from chronic facial and neck pain as well as recurring headaches. In some cases, this pain is due to Temporomandibular Disorder, or TMD.
Your temporomandibular joints (TMJ) connect your lower jawbone to your skull. These joints get a lot of use throughout the day as you speak, chew, swallow, and yawn. Pain in and around these joints can be unpleasant and may even restrict movement.
Symptoms Of TMD Include:
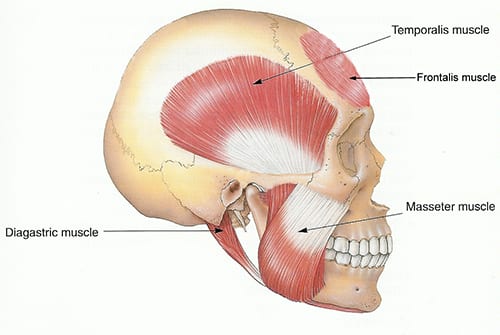
- Pain in the jaw area
- Pain, ringing, or stuffiness in the ears
- Frequent headaches or neck aches
- Clicking or popping sound when the jaw moves
- Swelling on the sides of the face
- Muscle spasms in the jaw area
- A change in the alignment of top and bottom teeth
- Locked jaw or limited opening of the mouth
Should you notice any of these symptoms, let your doctor know. Your dentist can help indicate the presence of TMD and create an effective treatment just for you.
There are a few simple steps you can take at home or work to prevent TMD from becoming more severe, or to prevent it from occurring:
- Relax your face — remember the rule: “Lips together, teeth apart”
- Avoid grinding your teeth
- Avoid constant gum chewing
- Don’t cradle the phone receiver between your head and shoulder — either use a headset or hold the receiver in your hand
- Chew food evenly on both sides of your mouth
- Do not sit with your chin rested on your hand
- Practice good posture — keep your head up, back straight, and shoulders squared
